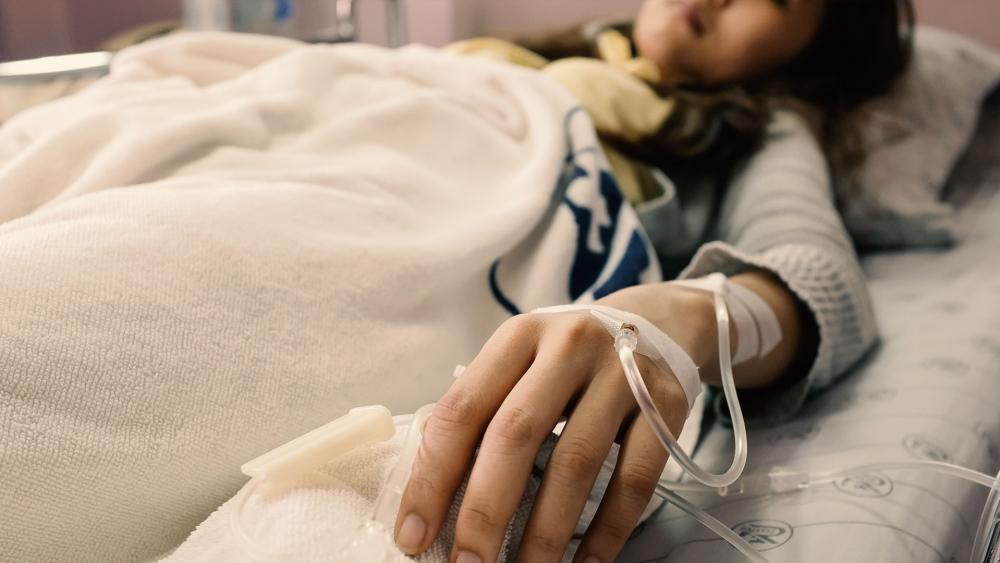
For many people, going to the hospital can make for an uneasy experience. First, patients and families worry about the illness or test they're facing. On top of that, there's the possibility of acquiring an infection during their stay.
Armando's Story
Armando Nahum knows what it's like for a loved one to become infected in a healthcare setting while being treated for a different reason. Sadly, he's probably seen it more than most.
"Three members of my family were impacted with hospital-associated infections at three different hospitals, in three different states, in ten months' time, culminating with the death of our son, Josh," Nahum told CBN News.
It began when Armando's father came down with pneumonia while hospitalized for bypass surgery. Then, during a stay for a different type of surgery, Armando's wife Victoria developed a staph infection. While those two survived their infections, Armando says his 27-year-old son did not recover, due to a sepsis infection he contracted after being admitted and treated for skydiving injuries.
"You always have a broken heart when you lose a child but it doesn't matter how old the child is," Nahum said.
On any given day, one out of every 31 patients has a healthcare-associated infection, according to the U.S. Department of Health and Human Services. These infections lead to tens of thousands of deaths each year.
Patients can acquire several different types of infections, such as viral, fungal, and bacterial while staying at hospitals or other healthcare settings including medical rehabilitation centers or nursing homes. Bacterial infections are the most common. According to the U.S. Centers for Disease Control and Prevention, urinary tract infections, bloodstream infections, and pneumonia are often associated with invasive devices such as catheters or central lines, and ventilators. Surgical sites can also become infected.
Hospital Response
In addition to the damage to the patient, these infections cost the healthcare system billions of dollars, according to Tracey Odachowski, Director of Infection Prevention and Control at Sentara Health.
"If a patient acquires an infection while in the hospital, then it's the hospital that pays that," Odachowski told CBN News. "The insurance company and Medicare will not."
Hospitals, such as Suffolk, Virginia's Sentara Obici, constantly look to reduce the risk. For example, after disinfecting rooms, advanced technology helps ensure they got rid of the bacteria. Workers take a surface sample by swabbing the area just cleaned, then inserting the swab into a reader that immediately analyzes the level of pathogens detected in the surface sample.
"Anything less than 250 is a pass, anything over 250 is a fail. My team will come back and re-clean the surface if it failed and re-test the surface again," Tory Kee, Sentara's Environmental Services Manager told CBN News.
***Please sign up for CBN Newsletters and download the CBN News app to ensure you keep receiving the latest news from a distinctly Christian perspective.***
Another disinfection practice involves saturating the room with ultraviolet C (UVC) light, which studies show can reduce by one-third, the transmission of three antibiotic-resistant bacterial infections, methicillin-resistant staphylococcus aureus (MRSA), C. difficile, and Acinetobacter.
Some hospitals now use copper to help fight infections, on hard surfaces like copper-infused over-bed tables, and even in linens, like bed sheets that have copper woven into them.
"Copper just has natural antibacterial properties to it," said Odachowski. "It helps kill any bacteria on site, so it's just an added layer of benefit to help prevent any infections."
Most healthcare workers understand the sooner a medical device is removed, the lower the risk of infection. Therefore, they regularly, sometimes daily, evaluate patients to determine how quickly a device can safely be taken out. They also closely watch patients for symptoms of an infection, like fever or diarrhea, and whether patients need to be tested for infection. The sooner one is identified, the sooner the patient can be isolated to stop the spread.
What Patients Can Do
While hospitals and other healthcare settings are taking steps to reduce infections, there's actually a lot of patients and their families can do, both ahead of time and during the stay.
The healthier a patient is before entering the hospital, the lower their risk. Experts say a big part of overall good health involves a robust gut microbiome. That means having good bacteria in the intestines, which can often fight off the bad bugs encountered at the hospital, especially those resistant to antibiotics, like C. diff. Patients are advised to ask their doctor whether antibiotics are truly needed, because these drugs tend to kill all bacteria in the gut, including the good.
"C. diff is in all of us naturally," Odachowski explained. "And if they're taking antibiotics that are not needed, it's going to kill the flora that's in your stomach that helps prevent C. diff from going crazy."
Odachowski advises family members who are taking a patient home from a healthcare setting, to resist the temptation to ask for a urinary catheter for the patient. Sometimes family members prefer this device because it often saves them the trouble of cleaning the patient, but urinary catheters are often the source of infection.
READ Eliminating 'Medical Deserts': Christian Ministry Partners with Health Care System to Reach Under-Served Populations
"There are times when it's absolutely necessary to have a urinary catheter," Odachowski said. "But as soon as that necessity has diminished, we need to get it out."
Armando's experience with hospital infections motivates him to help others as the co-founder of the Safe Care Campaign, an organization dedicated to working on early prevention and detection of all types of infections, whether they occur in a healthcare setting, in the community, or at home.
"Ask a lot of questions," he said. "Don't be afraid to ask a lot of questions, and certainly don't be afraid to ask the health care workers to wash their hands. It is the single most important component to the delivery of care, hand-hygiene, hand-sanitizing."
People who visit someone in a healthcare setting should also wash their hands to help prevent the spreading of disease.
"We touch our face so many times," Karen Zastrow, who works in infection control for Sentara Health, told CBN News. "We don't know what surfaces we've touched. You might get an itchy nose, itchy eyes. That's how most of the infections go into your body, through the mucous membranes."
Some hospitals have lower infection rates than others. If you have a choice, talk to your doctor about which facility is best for you, or consult "Hospital Compare" on the Medicare website.
READ Christian Homeless Clinic Results in 80% Drop of Unnecessary ER Visits
Did you know?
God is everywhere—even in the news. That’s why we view every news story through the lens of faith. We are committed to delivering quality independent Christian journalism you can trust. But it takes a lot of hard work, time, and money to do what we do. Help us continue to be a voice for truth in the media by supporting CBN News for as little as $1.











 Support CBN News
Support CBN News







